Endometriosis Fertility Solutions
Advanced management of endometriosis to restore fertility, reduce pain, and improve reproductive outcomes.
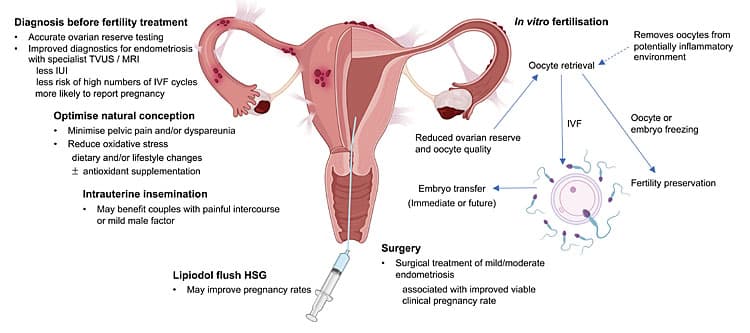
Endometriosis and Fertility
Endometriosis affects 10% of reproductive-aged women and is found in 30-50% of infertile women. It impacts fertility through anatomical distortion, inflammation, impaired implantation, and ovarian dysfunction.
Fertility Impact by Stage
- Stage I-II: 2-4% monthly fecundity (vs 15-20% normal)
- Stage III-IV: Natural conception rare without treatment
- Endometriomas: Reduce ovarian reserve by 30-50%
- Deep infiltrating: Significantly impairs tubal function
Comprehensive Treatment Strategies
Surgical Management
Laparoscopic Excision
- • Gold standard treatment
- • Complete lesion removal
- • Ovarian preservation techniques
- • Pregnancy rates: 40-60%
Endometrioma Management
- • Cystectomy vs drainage/ablation
- • Anti-adhesion barriers
- • Ovarian reserve preservation
- • Fertility preservation options
Medical & ART Approaches
Ovulation Induction/IUI
- • For minimal/mild endometriosis
- • 3-6 month trial
- • Pregnancy rates: 10-15% per cycle
- • Combined with GnRH suppression
IVF/ICSI
- • For moderate/severe endometriosis
- • Pregnancy rates: 45-55% per cycle
- • Long GnRH agonist protocol preferred
- • Embryo freezing for staged treatment
Treatment Outcomes
52%
Pregnancy rate after excision surgery
68%
Live birth rate with IVF after surgery
75%
Pain reduction after comprehensive treatment
Surgical Success Factors
- • Complete excision of all lesions
- • Adhesion prevention techniques
- • Ovarian reserve preservation
- • Multidisciplinary approach
Optimal Treatment Sequence
- Diagnostic laparoscopy with excision
- 3-6 months GnRH suppression
- 6 months timed intercourse/IUI
- Proceed to IVF if not pregnant
Endometriosis Expertise at DAARA
- Deep excision specialists
- Advanced laparoscopic/robotic surgery
- Ovarian reserve preservation techniques
- Multidisciplinary pain management
- Endometriosis-focused IVF protocols
- Fertility preservation counseling
- Recurrent endometriosis program
- Research and innovation center
Our endometriosis fertility program achieves 65% pregnancy rates within 18 months of treatment. Take control of your endometriosis and fertility journey.
Frequently Asked Questions
Should I have surgery before IVF for endometriosis?
For stage I-II: IVF can proceed without surgery. For stage III-IV with endometriomas >3cm: Surgery improves IVF outcomes and reduces infection risk. For deep infiltrating endometriosis: Surgery before IVF improves implantation. Our individualized approach considers symptoms, ovarian reserve, and lesion location.
Does endometriosis affect egg quality?
Yes. Endometriosis creates a hostile pelvic environment with inflammation and oxidative stress that can impair egg quality. Studies show higher DNA fragmentation in eggs from women with endometriosis. Antioxidants (NAC, CoQ10) and anti-inflammatory agents may help improve egg quality.
Can pregnancy cure endometriosis?
No, but pregnancy may provide temporary symptom relief due to progesterone dominance. Endometriosis often recurs postpartum. Comprehensive treatment during reproductive years provides the best chance for long-term management and fertility success.
How soon after surgery can I start fertility treatment?
After diagnostic laparoscopy: 1-2 cycles. After excision surgery: 2-3 months. After endometrioma surgery: 3-6 months (depending on size). We typically recommend 3 months of GnRH suppression before starting fertility treatments to suppress microscopic disease.
Is IVF successful with endometriosis?
Yes. With appropriate protocols, live birth rates per cycle are 45-55% for women with endometriosis vs 50-60% without. Using long GnRH agonist protocols, PICSI for sperm selection, and assisted hatching can optimize outcomes. Cumulative success rates reach 80-90% within 3 cycles.