Asthenospermia (Low Sperm Motility)
Asthenospermia is characterized by reduced sperm movement, with less than 40% of sperm showing progressive motility, significantly impacting fertility.
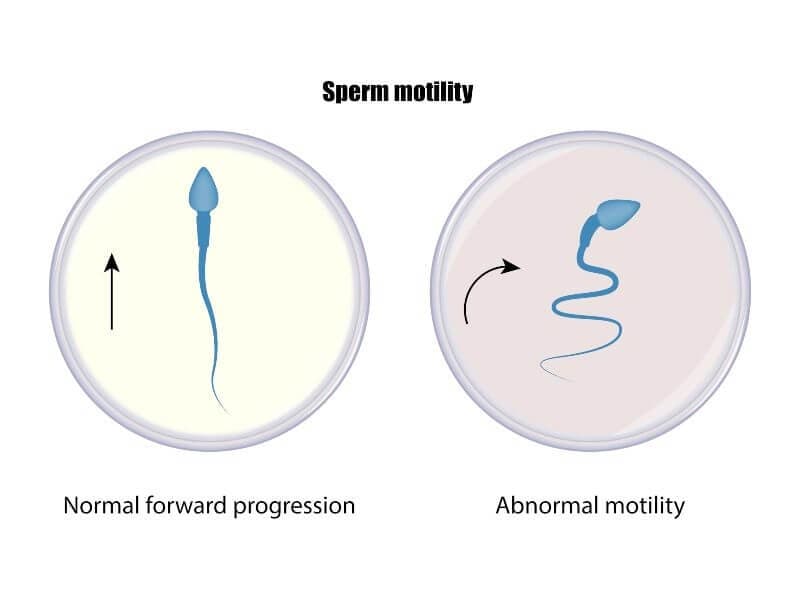
Understanding Low Sperm Motility
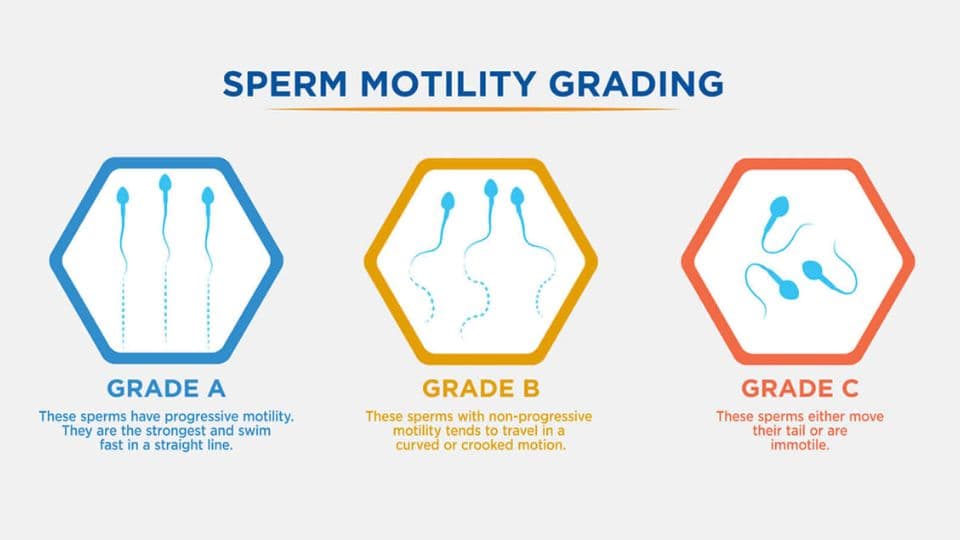
Asthenospermia refers to impaired sperm movement where sperm lack the progressive motility needed to reach and fertilize an egg. Motility is categorized as progressive (moving in straight lines), non-progressive (moving but not straight), or immotile. Diagnosis requires at least two semen analyses showing less than 40% motility.
Clinical Significance
- Affects 1 in 5 men seeking fertility treatment
- Reduces natural conception chances by 60-80%
- Often occurs alongside oligospermia (low count)
- Can be improved with targeted therapies

Causes of Low Sperm Motility
Oxidative Stress
- • Free radical damage to sperm
- • Imbalance of antioxidants
- • Environmental toxins
- • Poor diet and smoking
Structural Abnormalities
- • Defects in sperm flagella
- • Abnormal sperm heads
- • Genetic mutations
- • Kartagener syndrome
Medical Conditions
- • Varicocele
- • Infections (prostatitis, epididymitis)
- • Diabetes and metabolic disorders
- • Autoimmune disorders
Lifestyle Factors
- • Smoking and vaping
- • Excessive alcohol consumption
- • Obesity and poor nutrition
- • Exposure to heat and radiation
Environmental Toxins
- • Pesticides and herbicides
- • Heavy metals (lead, mercury)
- • Endocrine disruptors (BPA, phthalates)
- • Industrial chemicals
Genetic Factors
- • DNA fragmentation
- • Mitochondrial defects
- • Chromosomal abnormalities
- • Cystic fibrosis gene mutations
Advanced Diagnosis
Specialized Diagnostic Tests
CASA Analysis
Computer-Assisted Sperm Analysis
- • Measures progressive motility percentage
- • Analyzes swimming speed and patterns
- • Provides VCL, VSL, VAP parameters
- • Cost: $150-300
Sperm DNA Fragmentation
Assessment of DNA integrity
- • TUNEL assay, SCSA, Comet test
- • Evaluates oxidative damage
- • Predicts ART success rates
- • Cost: $250-500
Biochemical Tests
Seminal plasma analysis
- • Reactive oxygen species (ROS)
- • Total antioxidant capacity (TAC)
- • Fructose and zinc levels
- • Cost: $200-400
Ultrasound Imaging
Scrotal and transrectal scans
- • Varicocele detection
- • Ejaculatory duct evaluation
- • Testicular blood flow assessment
- • Cost: $200-350
Specialized Treatment Options
Antioxidant Therapy
3-6 months duration
High-potency antioxidant formulations to combat oxidative stress and improve sperm motility.
Key Supplements
- • CoQ10 (200-600mg/day)
- • L-carnitine (2g/day)
- • Vitamin C (1000mg/day)
- • Vitamin E (400IU/day)
- • Selenium (200mcg/day)
Treatment Protocol
- • Comprehensive antioxidant panel testing
- • Personalized supplement regimens
- • Dietary modification counseling
- • Progress monitoring every 3 months
Medical Treatments
3-12 months duration
Targeted medical approaches to address underlying causes of poor sperm motility.
Varicocele Repair
Microsurgical subinguinal approach
Antibiotic Therapy
For genital tract infections
Hormone Therapy
For endocrine imbalances
Assisted Reproductive Technologies
Sperm Preparation Techniques
Motility EnhancementAdvanced methods to select and enhance motile sperm for ART procedures.
- • Density gradient centrifugation
- • Swim-up technique
- • Magnetic activated cell sorting (MACS)
- • Microfluidic sperm sorting
ICSI (Intracytoplasmic Sperm Injection)
60-80% fertilizationDirect injection of a single motile sperm into the egg, bypassing natural motility requirements.
- • Ideal for severe motility issues
- • PICSI for physiological selection
- • IMSI for high-magnification selection
- • High success rates with viable sperm

Treatment Outcomes
Expected Improvement
Treatment Success Rates
- Antioxidant therapy40-50% motility improvement
- Varicocele repair60-70% improvement
- IUI with washed sperm15-25% per cycle
- IVF with ICSI60-75% fertilization
Recovery Timeline
- • Initial improvement: 2-3 months
- • Peak results: 4-6 months
- • Sperm regeneration cycle: 72-90 days
- • Regular semen analysis monitoring
Prognosis: Most men with asthenospermia see significant improvement with proper treatment. Even in severe cases, ART techniques like ICSI offer excellent chances of biological fatherhood.
Advanced Motility Treatment at DAARA
- Specialized andrology lab with CASA technology
- Advanced sperm DNA fragmentation testing
- Personalized antioxidant protocols
- Microsurgical varicocele repair expertise
- Cutting-edge sperm selection techniques
- High-success ICSI program
- Comprehensive lifestyle counseling
- Evidence-based treatment protocols
Schedule your motility assessment today. Our specialists will identify the underlying causes of your asthenospermia and create a personalized treatment plan to improve your sperm movement and fertility potential.
Frequently Asked Questions
What percentage of sperm need to be motile for fertility?
According to WHO standards, at least 40% of sperm should show progressive motility for optimal fertility. Values below 32% are considered abnormal.
Can sperm motility improve naturally?
Yes, lifestyle changes like quitting smoking, reducing alcohol, maintaining healthy weight, exercising, and antioxidant-rich diets can improve motility within 3-6 months.
How does varicocele affect sperm motility?
Varicoceles increase testicular temperature and oxidative stress, damaging sperm membranes and mitochondria which power sperm movement. Repair typically improves motility in 60-80% of cases.
Is IVF successful with low motility sperm?
Yes, with ICSI (intracytoplasmic sperm injection), fertilization success rates are 60-80% even with severe motility issues, as it bypasses natural sperm movement requirements.
What's the difference between motility and morphology?
Motility refers to sperm movement capability, while morphology describes sperm shape and structure. Both are important but independent parameters of sperm quality.